Wedding season again, already? I feel like we just got…

My Birth Story
When I tell my friends this story – after we get through all the horrible scary parts and a few fun gross TMI details – we get to the end where the baby and I are both okay and it feels appropriate to laugh a bit. At this point, they usually say something along the lines of “It was just so Emily of you to try to die in childbirth. Like something out of a Henry James novel or Downton Abbey.” They’re right, I have had a knack for landing myself in a good Edwardian saga (cf: being attacked by dogs in the French countryside last year). Very gratefully, this birth story doesn’t end up with a handsome widower and his darling daughter. Thank you, thank you to blood donors and doctors who saved my life!
Part I – The Quick and Painless Birth
Things would go wrong later, but for the actual birth I have a wonderful little jewelbox of a memory. On Monday, August 1, Rob and I went to the hospital for the regular non-stress test they give you when you’re a week overdue. The baby wasn’t moving around quite as much as usual and my contractions were seven minutes apart, so they checked me in to labor and delivery to be induced. Ate our first hospital breakfast tray in the triage ward before being moved to an antepartum room.
Jean came up on the train and the day went pretty quickly. At one point, we escaped to the roof garden and Jean made me laugh so hard I peed on the cement tile in full view of all the patient rooms around the courtyard. Rob went to the market and bought some ice cream for me to have after the baby arrived.
I was started on a whiff of pictocin after dinner. A nice nurse moved us into one of the fancy labor rooms before the ward got too crowded. Jean and Rob decorated it with Christmas lights, baby outfits and a lavender plant. At 11:30, we watched Stephen Colbert start his monologue and my water broke. I had maybe one or two “real” contractions – SO PAINFUL – before calling for the epidural. The anesthesiologist came almost immediately and I used all my yoga training to stay still while they administered it. Amazing pain relief right away. I could still feel my legs but everything else was turned off.
As they finished with the epidural, I had one long four minute contraction, started vomiting and the fetal distress monitors began beeping. All kinds of doctors and nurses rushed in and had me try different positions in the bed. I was happy to see my own pre-natal obgyn arrive – didn’t expect her to be on delivery. They rushed my bed off to the OR across the hall just in case they needed to do an emergency c-section. By the time we got there, the baby was stabilizing. I received a shot to stop the contractions and antibiotics. I remember feeling really cold and shivery but otherwise calm. They brought me wrapped in warm blankets back to the room where Rob had been dressed in scrubs just in case. I can famously power nap through almost anything and proceeded to do just that. Curled up under the blankets for an hour.
When the fetal distress started picking up again – I surprised everyone by having gone from 3 centimeters to 10 while sleeping and being ready to deliver this girl safely to the world. The room filled with doctors for me and the baby. I ate a few honey straws for energy and chatted with my doctor about her recent popular research study. The room seemed to shrink down to just my bed, lit with topaz colored lamps. Characteristic of big moments in our life like our wedding, Rob was nervous and serious and I was jazzed.
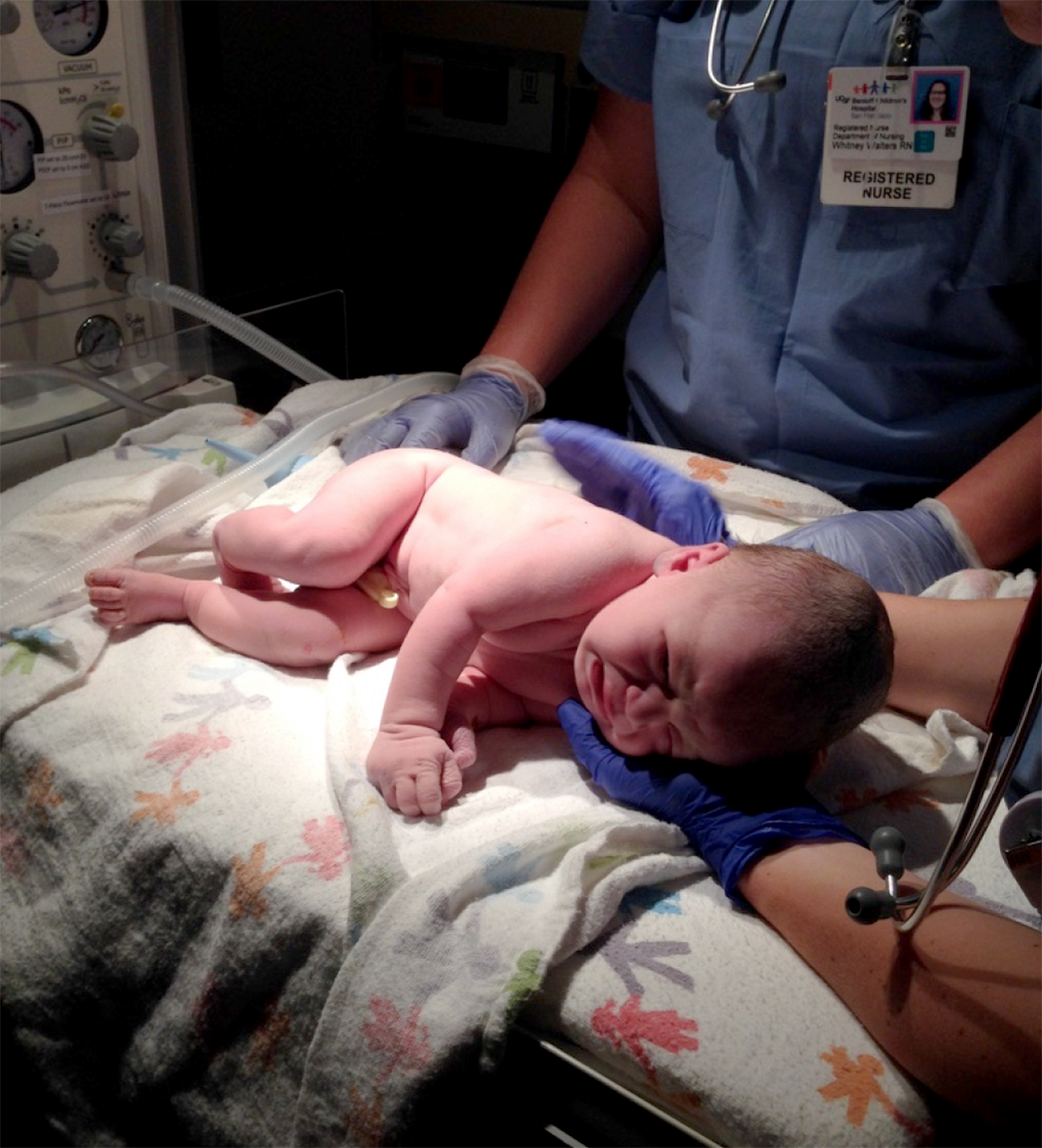
It was time to push. I used all my strength from yoga, all those months of braxton hicks contractions and all those five mile daily walks to bear down five times. One more with forceps to help and Lucille was with us at 4:18 am on the 15th anniversary of Rob and I first meeting.
I remember my sister making her trademark happy cooing noises and feeling so strong and proud. The pediatrician told me that the baby needed a little help with breathing but that she would be fine. I could see her healthy chest from my bed. Rob cut the cord. She was nearly 8lbs and 23 inches – with those long legs we were expecting.
I started to feel dizzy quickly after, like I was going to faint. I remember my doctor ordering a bunch of people around, Rob being by my side and then passing out.
Part II – The Worst Part
I’m glad I wasn’t there for this part. I hemorrhaged after delivery and for some reason my body went into full DIC shutdown – where your blood can no longer clot – within just a few minutes. They think that I might have been bleeding internally for a few hours before delivery. I was wheeled off to the OR and the baby off the NICU. Rob and Jean were left behind.
For five hours in the OR, I received 30 units of donated blood and platelets, a 2lb water balloon in my uterus and 16 feet of gauze packed in my birth canal. In hour six, I was taken to interventional radiology where they went through my femoral artery to insert a coil into the main blown out vein and then manually find and patch each of the other bleeding veins with bits of foam. About 30 doctors were involved in my care during all this.
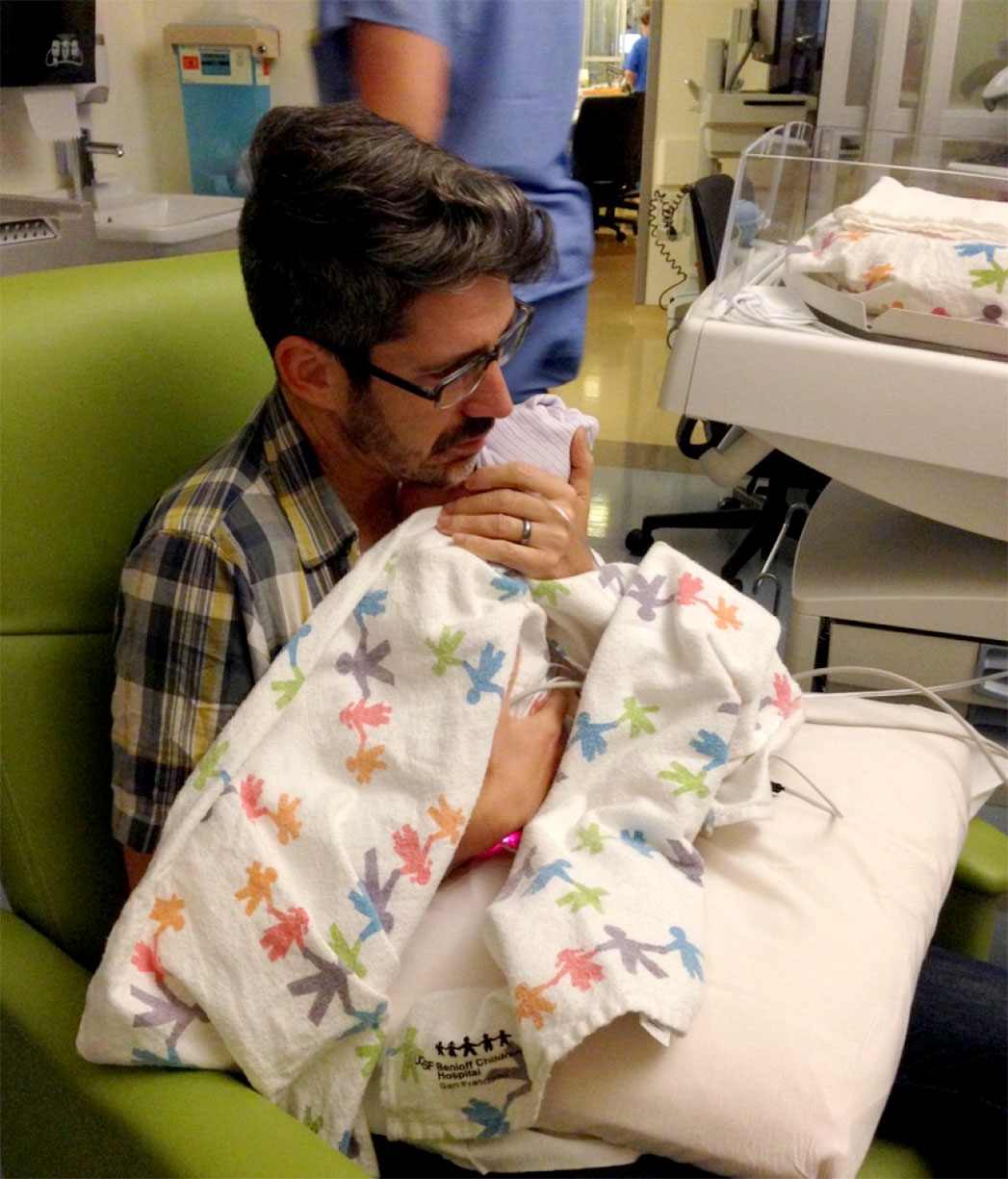
It was hard for Rob and Jean to get updates on my progress. They took turns sitting in the NICU with the baby as she got an IV of antibiotics and some help breathing after a bit of meconium and then chasing down nurses back on the labor and delivery floor. A lot of crying.
At 7:00, they called my Mother to drive up from Southern California and by 10:00 she got the report that I “going to make it.” She arrived shortly after and got to snuggle with Lucille in the NICU.
I was moved to the ICU at 11:00 and the plan was to keep me intubated for 48 hours. Lucille continued to do very well in the NICU and Rob was quickly learning all about baby care from the teams of experienced nurses. So gorgeous!
Part III – The ICU
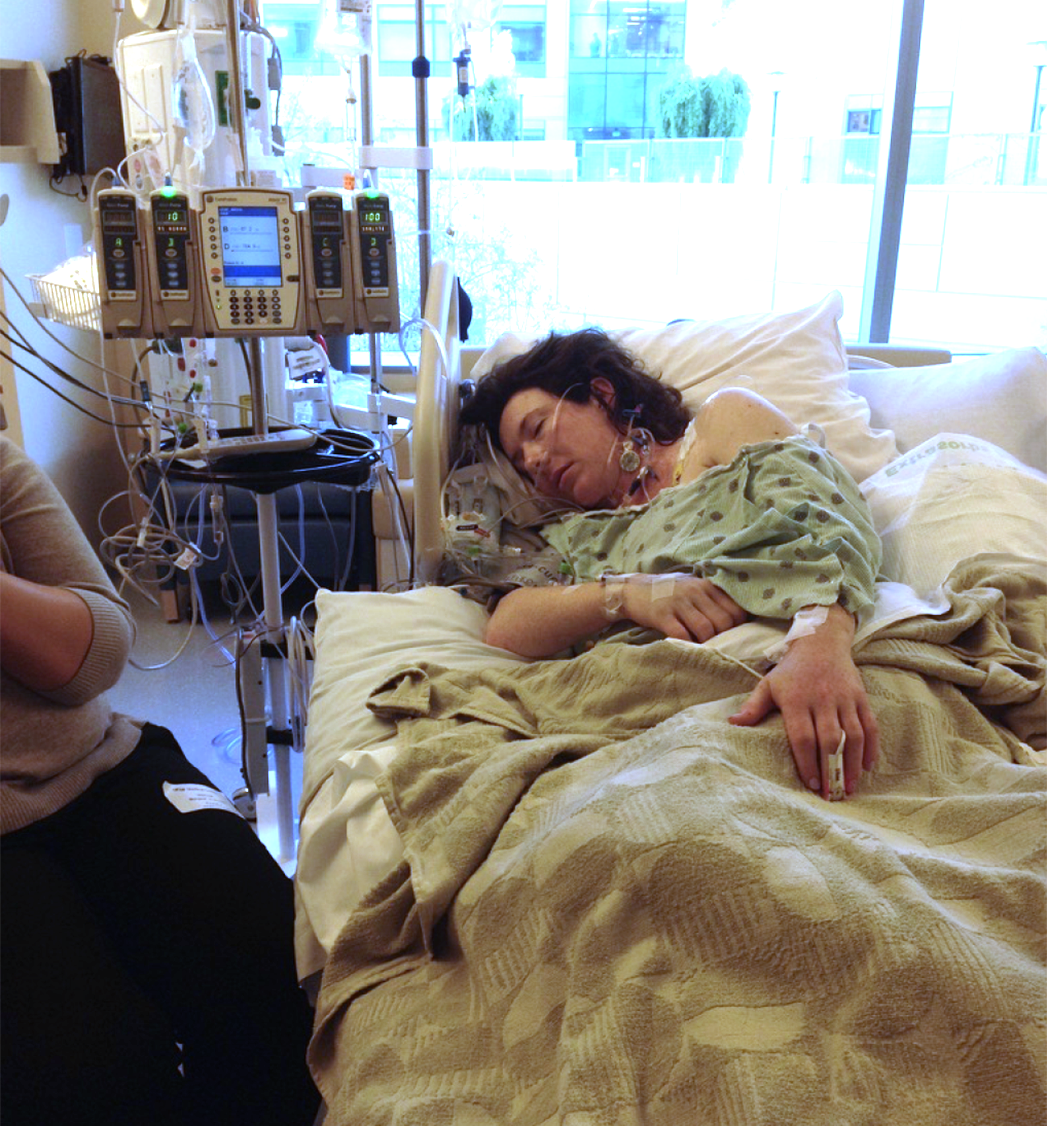
A lot of this is a blur for me. I was doing better than expected, so they took me off the respirator and woke me up after only six hours on Tuesday. I remember being so sure while waking up that I had a massive abdominal cut, but I was all in one piece. I had nine IVs, including two central lines, one on each side of my neck, going straight to my heart.
The amazing ICU nurses made my puffy and bruised body so comfortable with a nest of pillows – and a lot of narcotics. I remember sleeping in 30 minute stretches between the various alarms with the soothing whoosh of oxygen being jetted in through my nose and the cat-like massage of the circulation leg wraps on my ankles. Rob arranged for friends to come sit with me at night when the NICU closed to visitors and he went to take care of the baby.
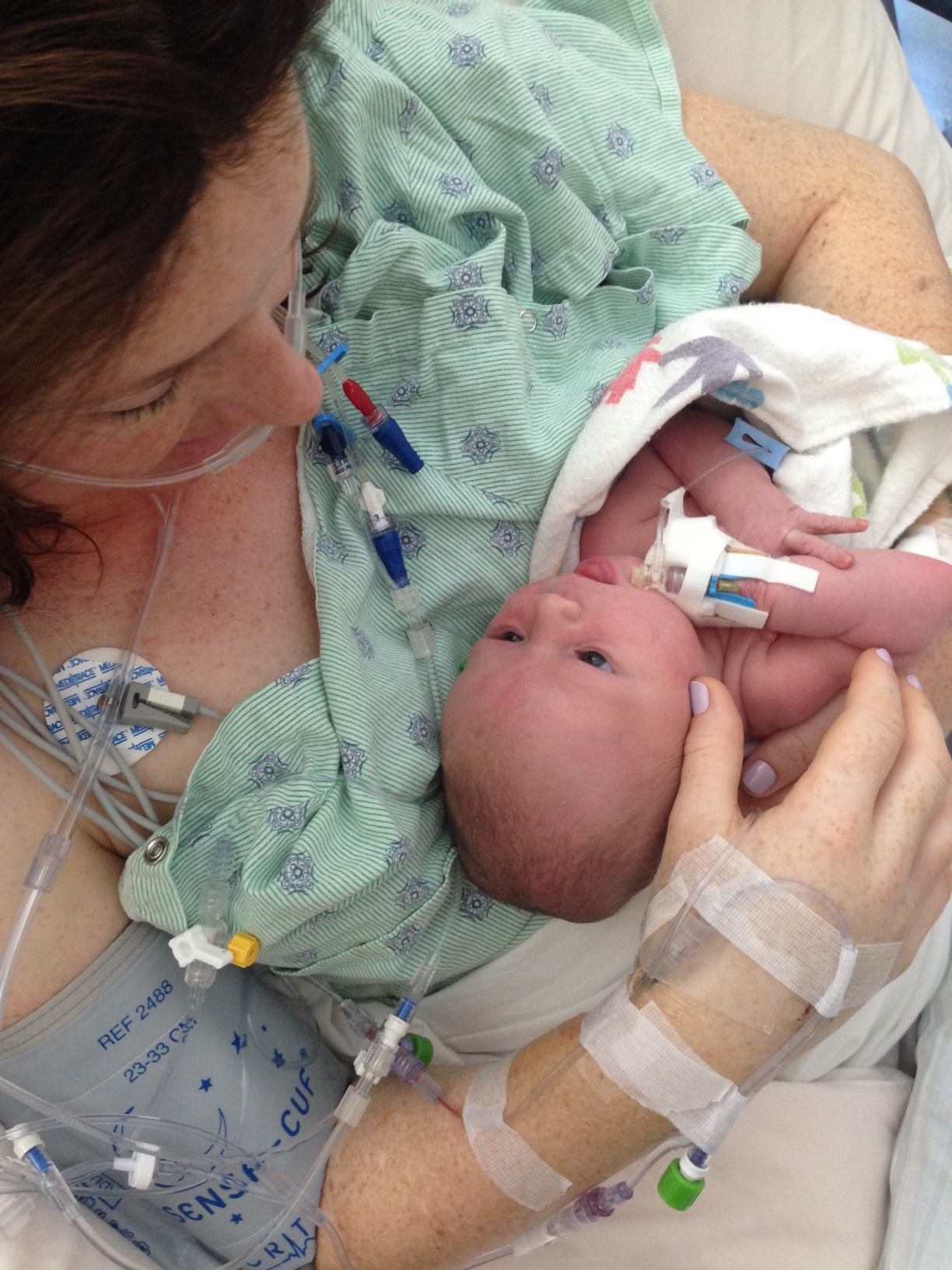
On Wednesday, a nurse brought Lucille up from the NICU to see me for the first time. It was lovely – even though I was getting another blood transfusion simultaneously. She nestled into my chest with our matching IVs and we both looked at each other like “oh hey, where have you been?”
After 10 months together, there was no question of recognition. She stayed for almost an hour, sleeping face down on my chest and claiming me as hers, before they took her back to her floor.
Most of my ICU stay involved three things – 1) taking things out, including IVs, the balloon and gauze, 2) tiny milestones like being able to move from ice chips to water to clear liquids and 3) a parade of shellshocked doctors who visited my bed to say they were part of the team that worked on me and I think to check that I really was alive. I remember feeling drunk with responsibility when they set me up to brush my own teeth.
On Thursday, Lucille was due to be discharged from the hospital and I was still in the ICU. Rob fought a heroic battle with various nurses and doctors in different departments to make sure we could all stay together in the hospital. The chief pediatrician was adamant that the baby be sent home with a hired doula. Rob had to assemble his own 24-hour baby care team and present them for approval before the doctor would relent to let her stay. The ICU team also rallied to help, coordinating with post-partum to move me downstairs early to a family room to continue my recovery. Poor Rob. Labor might have almost killed me, but hospital bureaucracy almost killed him that day.
Part IV – Post-Partum
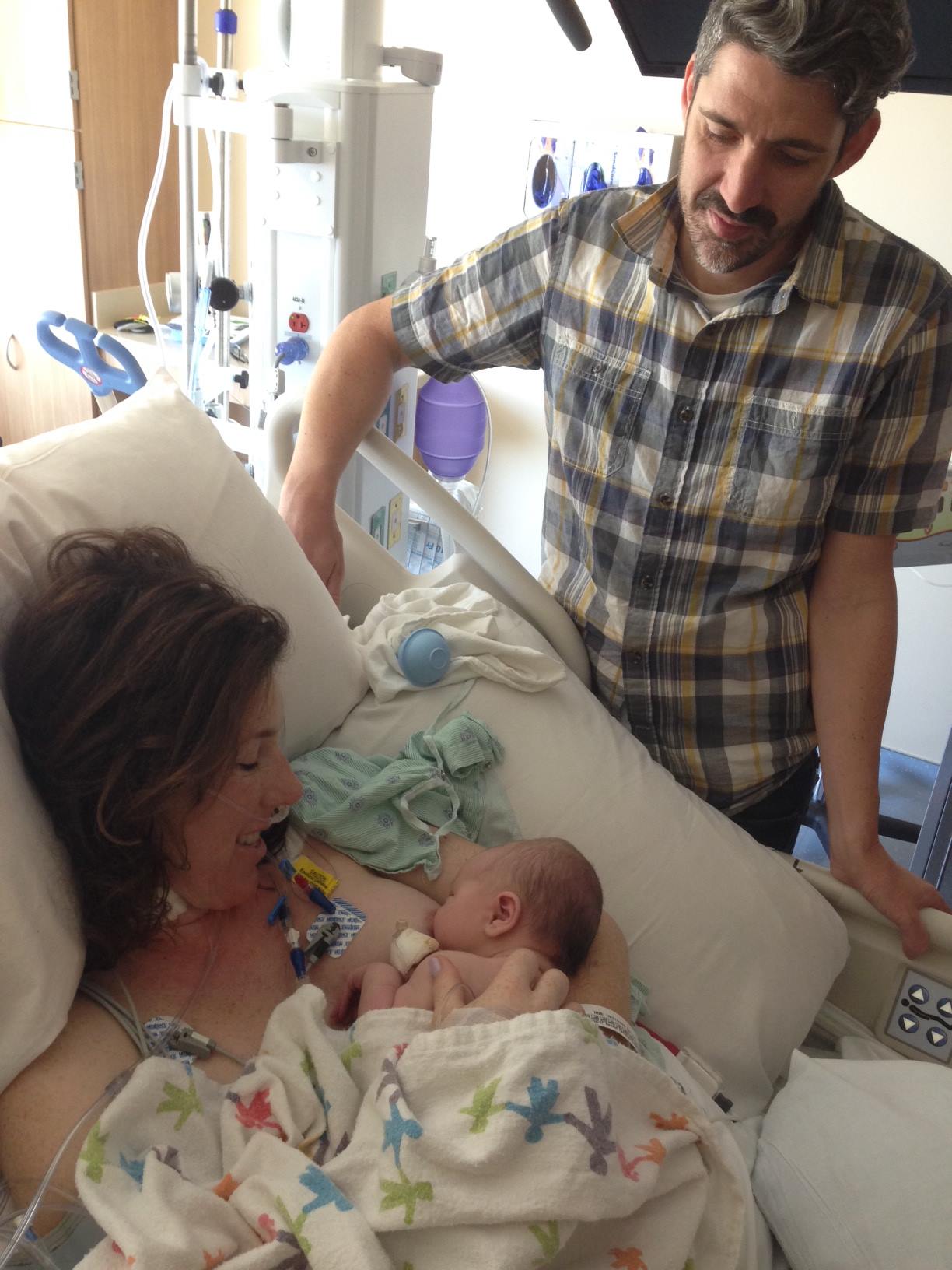
At 6:00 on Thursday we had a grand reunion on the post-partum ward. Rob got the baby discharged from the NICU first.
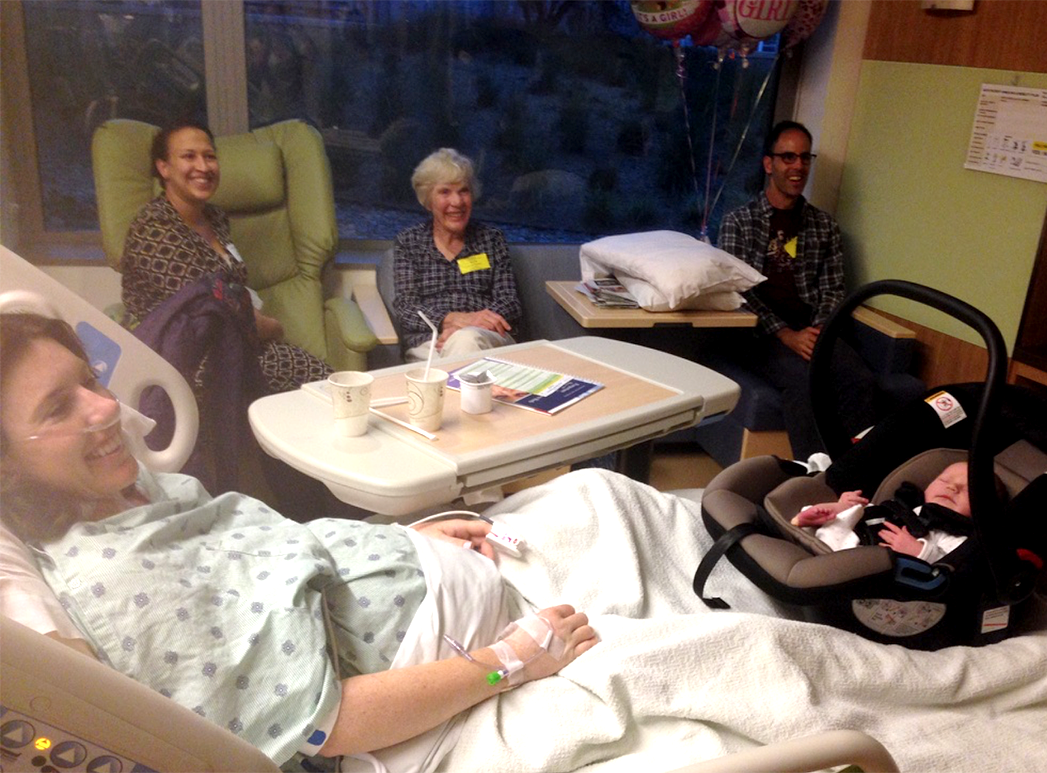
Then, they moved me from the ICU to a room right across from the nurses station. We were overjoyed to be all together with baby and friends for the first time. The amazing nurses acted quite pleased to see me, but in reality I must have been so, so much more work for them these first few days. It was a strange feeling to “drive” my own body outside the ICU that first night.
I couldn’t walk, still had a catheter and couldn’t hold the baby for more than a minute even with supervision – but I could work my professional charisma hard from the bed to charm all my nurses. By the end of each 12 hour shift, I knew each of their life stories. I worked hard to be their favorite patient and they loaded me up with extra Cushing’s Cream for my hemorrhoids (three ingredients: cocaine, morphine and zinc oxide) and gave me the royal treatment. Like Rob kept saying, the only thing you can control in this kind of situation is your attitude. I felt truly and honestly grateful for every milestone.
Those next four days in the hospital were happy for me. Room 14 became our new apartment. Rob rallied our friends from far and wide to help. Mom came every day from 7:00 to 3:00. Margaret, Alison, Jackie, Rich and Yvonne came for four hour shifts in the evening to hold and feed the baby while Rob took naps on the fold down bed.
Rob was too sleep deprived to drive so our friend Mark took him to the baby’s first pediatrician’s appointment across town.
Shane drove up from San Luis Obispo to help for an eight hour shift. He took Rob for a much-earned beer at a patio restaurant next door with Lucille.
Matt helped Rob shuffle supplies and people back and forth from our house. Rob hired a private night nurse to come from midnight to 4:00 am so he could sleep and Jean came to spend the night one time when the nurse couldn’t. We all did a lot of ordering Rob to “go back to bed” in those nights. Lucille was so helpful being an easy eater and sleeper – tucked away in her pram in the corner.
I have a gorgeous memory of watching from my hospital bed as Rob, backlit in the middle of the night, changed her diapers and washed bottles. The only thing we could see out the window beyond the garden was the occasional life flight helicopter or tourist sea plane flying by. It felt like we were on a ship far out in the ocean.
Meanwhile, I worked on getting my last few IVs out, my platelet count stabilized, kidneys back online, blood pressure down, pulse ox up, sleeping, taking a first few tentative walks to the bathroom and then to the end of the hall. My catheter was removed, and then after I peed gloriously all over the floor, put back in for a few more days. The nurses started to run out of veins for twice a day blood draws and we worked together to hunt for just one more each time.
Rob and a nurse helped me take my first shower, still not able to stand – and it was a religious experience. I learned how to make my own “chucks” diapers. My one task to help everyone else was ordering loaded meal trays from the cafeteria to be delivered three times a day to feed us. Our amazing insurance company CareFirst tracked me down and called the room to make sure I was okay and said that they would take care of everything.
By Sunday, I was well enough that I could do a lap around half the ward and my bone marrow was producing platelets again on its own. My blood started to look like real blood and not raspberry sorbet when they drew it. I felt like I had mostly caught up to the other new moms arriving on the floor. The catheter came out one last time. They talked about sending me home, but I did my best to seem poorly and hid from the nurses to get an extra night. We finally remembered the ice cream Rob bought on Monday – miraculously it was still in the freezer. Rob lost it when I finally got to dig in.
On Monday, they prepared to really send me home. A stressful day with visits from doctors and lactation consultants – but we were very ready to leave exactly a week after we had arrived.
That week felt like a lifetime. It was scary and terrible in a lot of ways but also gave us the gift of perspective and gratitude for the new lifetime we have ahead with Lucille.
(PS: Donate blood!)
Previous Post: Dear Lucille – Month One
















Wow. Such a scary story, but what a happy ending! I have followed your blog for ages and was a little worried when all went silent. I hope you are both doing well! Lucille is gorgeous.
Thanks Dee!
Congratulations, Emily!! I have been reading your blog for nearly ten years and am so happy for you and your family, and happy that you pulled through such a difficult post-birth experience. Wishing you, Rob, and your beautiful daughter all the best.
Thanks Cynthia!
Your story made me cry and smile and feel anxious and happy and basically all the feels. I’ve been reading your blog for a few years now. I am so glad you are such a fighter and that both you and Lucille are doing well. I wish you so much love and happiness!
It does cover pretty much every feeling, right? Thanks for the well wishes, Katie!
Wow! That is just about the most harrowing birth story I have ever heard. So glad you are fine now and get to spend time with your beautiful baby girl. What a lovely support system you have! Wishing you all the best in your recovery and with your new life as a mom!!!
Thanks Lark!
What a harrowing experience! Glad everyone’s okay. Lucille is gorgeous. 🙂
Thanks Jenny!
Omg. I, like you, had two ridiculous birth experiences. I now know I would not have lived in Elizabeth Bennett’s time or even in “And The Ladies of the Club’s.” It is okay. Modern times and modern medicine rock! Rest and keep accepting help.
Hooray for the 21st century 🙂 Glad you made it through too!
Oh Emily…..WHAT a birth story! My eyes filled with tears several times for you and Rob and Lucille. Your best days are ahead of you! Take care and congratulations! Love and prayers from Florida, Heather
Thanks Heather!
Emily, I don’t know you, but right now I am thanking god for modern medicine. You look amazing.
Thank you for the well wishes!
Wow. That is one heck of a story. So glad it had the ending it did. My 2nd baby was born by planned Cesarean because I had placenta previa (placenta covering the cervix). I was very humbling knowing that my baby and likely I would have died had we not had access to a clean and safe hospital. So many women don’t have this; it’s heartbreaking. Lucille is gorgeous! Have fun being amazed by her every move!
So glad you had that early intervention, Jill!
Wow! What an amazing story of medical prowess, devotion of family and friends, and LIFE! Blessings to you and yours – so very happy that baby Lucille is here at last and that you all are well. Hope you are following all that good advice about resting when the baby rests – or just resting!
Thanks Melissa!
Oh, Emily! Such a scary story- totally made me cry. I am so glad that you and the baby (and Rob) are ok. Sending you hugs and love.
Thank you so much for writing this Emily! All my questions were answered, and MORE!
That quote in the first paragraph (“So Emily of you to try to die in childbirth!”) sounded very Sarah-like to me!
So relieved for the happy ending!!! <3
Thank God for modern medicine! What a scary experience– Rob must have been terrified! So glad to read you’re doing well now. ..continue to rest and take it slowly. Lucille is truly one beautiful baby! Hugs to all.
P.s. I had placenta previa with my second pregnancy and remember the dire warnings from by OBGYN of “both you and the baby could die” if I started bleeding again. Yikes! I tried to follow his instructions carefully (no stairs , no intercourse, no,lifting), the last of which was tricky with a toddler running around. But, as my mom likes to say, “All’s well that ends well.” Blessings on you and your new family!
Thanks Susan!
So glad you all made it through this ordeal. Do they have any idea why this occurred? I mean, seriously, Emily, you will go to great lengths for a good story but this is beyond the pale. You have a gorgeous daughter and a wonderful extended family. You must feel so blessed. ❤️❤️❤️
Thanks Cathy! I do feel blessed.
Wow! Now I have something new to worry about for my delivery in about a months time. 😉
I was induced during my first pregnancy and while I wouldn’t describe it as quick and painless, it now seems so simple and complication free by comparison.
It’s nice to see you back and I hope your recovery has not interfered with getting lots of naked, newborn snuggle time!
What happened to me is super, super rare – I’m sure you’ll do great with your second labor! Just take good care of yourself 🙂
What a birth story! Congratulations to all three of you, and Lucille is a beautiful baby!
Thanks Natasha!
Oh Emily! My goodness, as a long time reader I was concerned when I read your last post. I’m so happy that you’re both healthy! Wishing you all the best! She is beautiful!
Thanks Cari!
Emily!!! Oh my goodness, my heart melts for you and your beautiful family. I got so teared up reading this. Thank you for sharing. I’m so very grateful and happy you pulled through! I cannot even begin to imagine the amount of strength and courage those long days in the hospital took. You are absolutely amazing…god bless you, Rob, and adorable little Lucille!
Thanks Kristin!
Wow! That’s all I can say. Rob is a hero, as are you and all your friends. Thanks for sharing. Blessings to you all!
Thanks Susan!
I’m so glad you’re okay.
Thanks Michele!
Dear Emily,
I have loved reading your blog over the years. I love how you and Rob always take care of each other on your grand adventures. What amazing training you’ve had in preparation for this grand adventure!!!
May you, Rob, and now sweet Lucille be continually blessed and watched over.
Much love from Arizona,
Sarah
Thanks Sarah!
This made me cry, of course–I’m so so glad you are ok. It’s amazing how invested in a person and their family you become after reading their blog for a decade! Thank god for modern medicine.
Side note: I didn’t put the dates together before, but Lucy and my Ellie share a birthday, four years apart. (My husband swears I held E in until 1 am on 8/2 so she wouldn’t born on *my* birthday, 8/1!)
A very auspicious week to be born! I hope we can find a way to meet on all our travels one of these days.
Me too!
Thank you Emily for writing this! It answered all my question, and even MORE!
I am so relieved that your story had a happy ending, and that you and Lucille, and Rob,
are well!
When I read your first paragraph, I was suspicious that quote sounded very much like Sarah!
(It is so Emily of you to try to die in childbirth!”)
Sarah was certainly one of the people who shared that comment!
Oh Emily! I ‘m an RN so I understand what you’ve been through. Like others have said, I’ve never met you but have read your blog for ages, so I felt emotionally invested in your pregnancy journey. I am so, so glad for your happy ending. Blessings to you and your family! Lucille is a beautiful and lucky girl to be born to such loving, strong parents. Also, the photos of your friends/extended family holding Lucille? So adorable!
Best,
Annie
Thanks Annie! I’m a HUGE fan of nurses now. Thanks for all your hard work!
I’ve been reading your blog for about 8 years now. My, that was a frightening story. I’m sorry you had to go through all that, but so glad to hear a positive outcome. I hope you are feeling stronger and healing well and that you and Rob are enjoying your sweet baby girl!
All the best,
Heather
Thanks Heather!